Sexually Transmitted and Bloodborne Pathogens Infection Rates in PEI
The Chief Public Health Office is mandated by the Public Health Act and the Notifiable Diseases and Conditions and Communicable Diseases Regulations to control certain communicable diseases in PEI. The Communicable Disease Program contributes to this mandate through policy development, disease surveillance, case follow-up, contact tracing, immunization, education and reporting on STBBI rates.
Sexually Transmitted and Bloodborne Infections
NOTE: The COVID-19 pandemic impacted both the provincial capacity to test for sexually transmitted and bloodborne infections (STBBI) as well as STBBI test-seeking behaviours of individuals.i The Chief Public Health Office urges caution when interpreting trends of STBBI infection rates, especially during the years 2020 to 2022.
Number of Diagnosed Cases and 5-year Moving Average Rate per 100,000 Population, PEI 2019-2024.
Number of Cases per Year
| 2019 | 2020 | 2021 | 2022 | 2023 | 2024 | |
| Chlamydia | 404 | 331 | 332 | 335 | 415 | 419 |
| Gonorrhea | 18 | 14 | 18 | 21 | 28 | 23 |
| Hepatitis B | 24 | 17 | 16 | 13 | 22 | 16 |
| Hepatitis C | 52 | 34 | 28 | 36 | 24 | 33 |
| HIV | 0 | 4 | 4 | 5 | 2 | 5 |
| LGV | 0 | 0 | 0 | 0 | 0 | 0 |
| Syphilis (Infectious) | 3 | 2 | 2 | 6 | 6 | 9 |
5-years Moving Average Rate
| 2019 | 2020 | 2021 | 2022 | 2023 | 2024 | |
| Chlamydia | 232.4 | 228.1 | 222.1 | 217.9 | 220.2 | 225.0 |
| Gonorrhea | 10.4 | 10.5 | 12.1 | 12.4 | 13.2 | 13.9 |
| Hepatitis B | 14.0 | 11.9 | 11.2 | 10.0 | 9.8 | 9.8 |
| Hepatitis C | 25.2 | 24.5 | 21.3 | 18.4 | 17.8 | 17.9 |
| HIV | 3.2 | 3.6 | 2.9 | 2.4 | 2.3 | 2.3 |
| LGV | - | - | - | - | - | - |
| Syphilis (Infectious) | 1.5 | 1.6 | 1.7 | 2.5 | 2.9 | 3.7 |
Rates were not calculated for 5-year rolling case counts less than 10
HIV: Human immunodeficiency virus
LGV: Lymphogranuloma venereum
Chlamydia
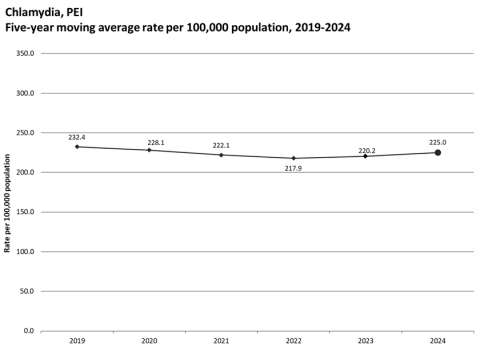
PEI – Chlamydia is the most commonly reported sexually transmitted infection in PEI. In 2024, the rate of chlamydia infections in PEI was stable at 225.0 cases per 100,000 population, and this rate was not statistically different from the average rate in the most recent five years prior (i.e., from 2019 to 2023). Chlamydia is often underdiagnosed because the majority of infected individuals are asymptomatic.
Canada – Chlamydia is the most commonly reported sexually transmitted infection in Canada. Between 2012 and 2019, national rates of reported chlamydia cases steadily increased annually (the 2019 chlamydia rate was22% higher then the 2012 rate) and remained stable between 2020 and 2021. In 2021, 104,426 cases of chlamydia were reported across the country for a rate of 273.2 cases per 100,000 population.
Gonorrhea
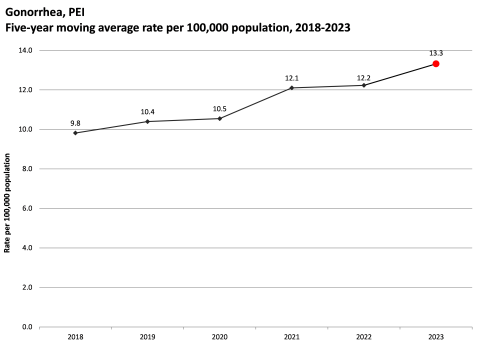
PEI – The rate of gonorrhea in PEI has been slowly increasing since 2013. In 2024, the rate of gonorrhea was 13.9 cases per 100,000 population, and this was more than double the rate reported in 2013 (5.8 cases per 100,000 population).
Canada – In Canada, gonorrhea is the second most commonly reported STI after chlamydia. Of particular concern is the emergence of antibiotic-resistant gonorrhea. Gonorrhea rates have increased by 124% over the past decade in Canada. In 2021, 32,192 cases of gonorrhea were reported nationally, corresponding to a rate of 84.2 cases per 100,000 population and this is double the rate reported in 2012.ii
Hepatitis C
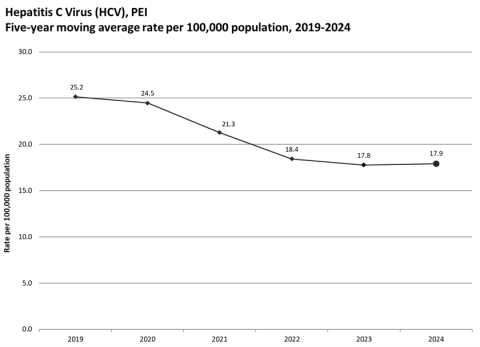
PEI – In 2014, PEI embarked upon a progressive approach for eliminating hepatitis C virus (HCV) that includes encouraging testing for individuals at high risk and providing new treatments through the Hepatitis C Drug Program. Since the implementation of the program, HCV⸸ rates have been declining and from 2018 to 2023, the rate dropped by 33%. In 2024, the rate of HCV infections in PEI was 17.9 cases per 100,000 population and this rate was not statistically different from the average rate in the most recent five years prior (i.e., from 2019 to 2023).
Canada - In 2021, 7,535 cases of hepatitis C were reported across the country for a rate of 19.7 cases per 100,000 population. From 2012 to 2018, national hepatitis C rates rose by 15.4% (from 29.4 to 33.9 cases per 100,000 population). However, from 2018 to 2020, the national rated dropped by 42.8% (to 19.4 cases per 100,000 population). More recently from 2020 to 2021 the rate of HCV increased slightly by 1.5%. iv
Hepatitis B
Hepatitis B virus (HBV) infections are classified as acute or chronic infections. National rates are influenced by variations in which each province distinguishes HBV cases by infection status. In 2021, there were 114 reported acute hepatitis B cases were reported in Canada for a rate of 0.30 per 100,000 population. National acute hepatitis B rates are low and have plateaued since 2010, with annual case counts remaining under 200.v Many provinces and territories implemented a universal HBV immunization strategy in the early 1990s aimed at infants and children, and this strategy is attributed with reducing acute HBV infections in this population. Additional decreases in rates may be achieved through improving immunization strategies for immigrants, refugees, and adopted children from countries without mass HBV vaccination programs.
HIV
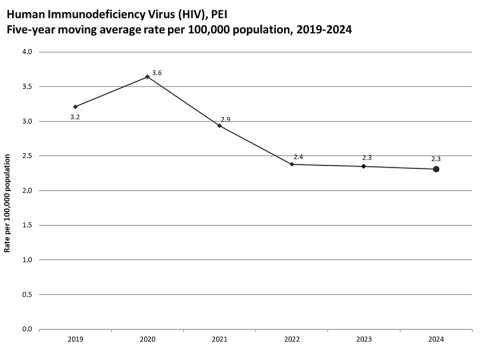
PEI – In PEI, we typically see between 0 to 2 local HIV transmissions per year, and many cases of HIV diagnosed in PEI resulted from an exposure that occurred outside of Canada and are not reflective of domestic transmission. In 2024, the rate of new HIV infection in PEI was 2.3 cases per 100,000 population, and this rate was not statistically different from the average rate in the most recent five years prior (i.e., from 2019 to 2023).
Canada - In 2023, 2,434 new diagnosed cases of HIV were reported which is a 35.2% increase since 2022. The national rate of new HIV diagnoses for 2023 was 6.1 cases per 100,000 population.
Syphilis (Infectious)
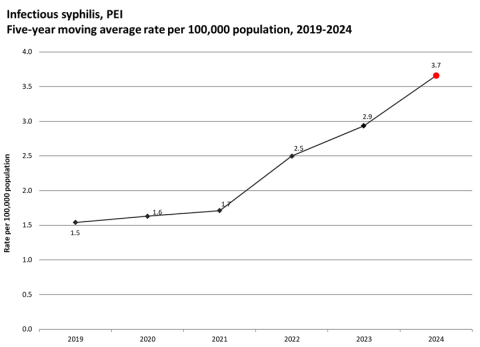
PEI – The rate of infectious syphilis in 2024 (5-year average rate of 3.7 cases per 100,000 population) was significantly higher than in the most recent five years prior. While the incidence remains comparatively low in PEI compared to rates observed in many other jurisdictions, ongoing and regular monitoring is important to detect further increases.
Canada - An increasing trend has been observed nationally as well and with a much higher incidence. In 2021, the rate was 30.2 cases per 100,000 population, and this rate was five times higher than the rate in 2012 (5.9 cases per 100,000 population). Rapidly rising rates among reproductive-aged females have led to an increase in the number of reported cases of babies born with congenital syphilis in Canada.ii
Notes:
Reported rates are five-year centred moving averages. A five-year centred moving average for a specific year is the average of the data from two years prior to that year, the specific year, and two years after that year. Moving averages are used to smooth the fluctuations in rates in order to make trends more apparent and to aggregate data with small cell counts. As a result of the methodology, the rates for the last two years of the study period (i.e., 2023 and 2024) are based on less than five years of data and are more heavily influenced by the historical data.
What are we doing?
- STI and STBBI testing at physician and nurse practitioner offices and at Health PEI Sexual Health Clinic, Options and reproductive Services (SHORS)
- UPEI Health & Wellness Centre(link is external) and Holland College health clinics are open for students 5 days/week and offer STBBI testing
- Development of STI education material and collaborating with community groups for increasing public awareness, specifically for populations at higher risk for STBBIs
- Prevention is provided with
- coverage for HIV Pre-Exposure Prophylaxis (PrEP) and Post-Exposure Prophylaxis (PEP) through the HIV program,
- the needle exchange program provides clean supplies for drug use to help prevent transmission of Hepatitis C, and
- Hepatitis B immunization is available through the childhood immunization program and through the adult immunization program
- Medication for those diagnosed with an STBBI is covered under the STI Drug program, the Hepatitis C treatment program and the HIV program
- All people who are infected with an STBBI are provided confidential follow-up with a Public Health Nurse. This follow-up includes education and assessment for immunizations that the person may require.
- In late 2022 the PEI STBBI Reduction Action Plan was released.
- A range of actions and related work has occurred over the past two years. The PEI Sexually Transmitted and Blood Borne Infections Reduction Action Plan Report summarizes the work that was undertaken which was based on the goals of the action plan.
References
i Public Health Agency of Canada. Survey of the impact of COVID-19 on the ability to provide STBBI prevention, testing and treatment including harm reduction services in Canada. PHAC. 2021.
ii Public Health Agency of Canada. Chlamydia, gonorrhea and infectious syphilis in Canada: 2021 surveillance data (infographic). PHAC. 2023
iv Public Health Agency of Canada. Report on Hepatitis C in Canada: 2019. PHAC. 2023.
v Public Health Agency of Canada. Hepatitis B in Canada: 2021 surveillance data update. PHAC. 2023
vi Public Health Agency of Canada. HIV in Canada: 2023 Surveillance Highlights. PHAC. 2024.
